What is congenital heart disease (“CHD”)?
Congenital heart disease exists when there is a defect in the structure of the heart which is present at birth. This causes blood to flow through the heart in an abnormal way, causing the heart muscle to strain and, ultimately, fail.
Symptoms frequently present early in life, but it is possible for some CHDs to go undetected for longer periods. It is a spectrum of disease whereby some children may show no outward symptoms, while others exhibit shortness of breath, cyanosis (turning blue due to oxygen deprivation), syncope (collapse), heart murmurs, under-development of limbs and muscles, respiratory infections, and poor growth.
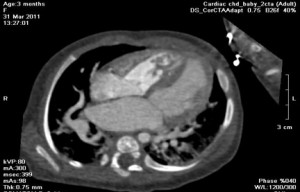
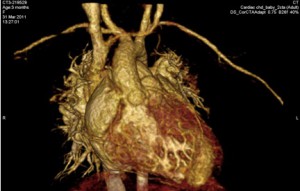
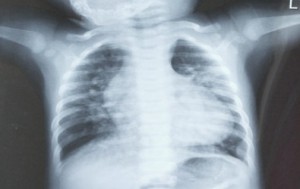
Tongtong suffered from a condition known as Tetralogy of Fallot. This is a congenital heart defect which classically involves multiple life-threatening anatomical abnormalities. It is one of the most common cyanotic heart defects, and the most common cause of ‘blue baby syndrome’. It was described in 1672 by Niels Stensen, and in 1888 by the French physician Étienne-Louis Fallot, after whom it is named.
Expected survival (if left untreated) is less than 30% at age ten, yet the condition is entirely treatable with today’s technology and medical expertise. In the best cardiothoracic centers, surgery is now often carried out in infants one year of age or younger, with more a greater than 95% post-operative success rate. The best long-term results are achieved when access to surgery is available before the development of heart failure.
Why do CHD patients in China need our help?
With vast urban migration over the past 20 years, the existing systems of healthcare insurance (based on a series of residency permits) are often limited by access and geography. Alternative provision by private healthcare is prohibitively expensive for the average family.
Modern congenital cardiac care is truly a collaborative team effort. It requires sophisticated diagnostic and monitoring equipment, highly trained nursing and technical support staff as well as skilled physicians and surgeons. It also requires a vast and complex hospital infrastructure to support a village of people to attain these capabilities.
State-of-the art care involves accurate diagnosis in the neonatal period or at least in early infancy; followed by early surgical repair. This approach has been clearly demonstrated to minimize the secondary deleterious effects of the cardiac problem.
One of the more tragic aspects of congenital heart disease is that it usually strikes young families at a stage in their lives when they are not well equipped financially to deal with the costs of cardiac surgery. Indeed, the complex medical expertise and urgent surgery required to correct these cardiac conditions can be so distant and expensive as to be completely out of reach of the vast majority of such families in our society.
Aside, from significant difficulties in gaining the best quality healthcare, and access to expertise and financial support, there is often also a limited and poor understanding amongst patient-relatives. They are thus unable to help themselves.
Hence there is need for a trusted platform to act as advocate and provide appropriate resources; using central coordination and the leverage of an extensive network of social contacts / technical expertise – to raise necessary funds, screen professionals and gain access to the best medical centers.